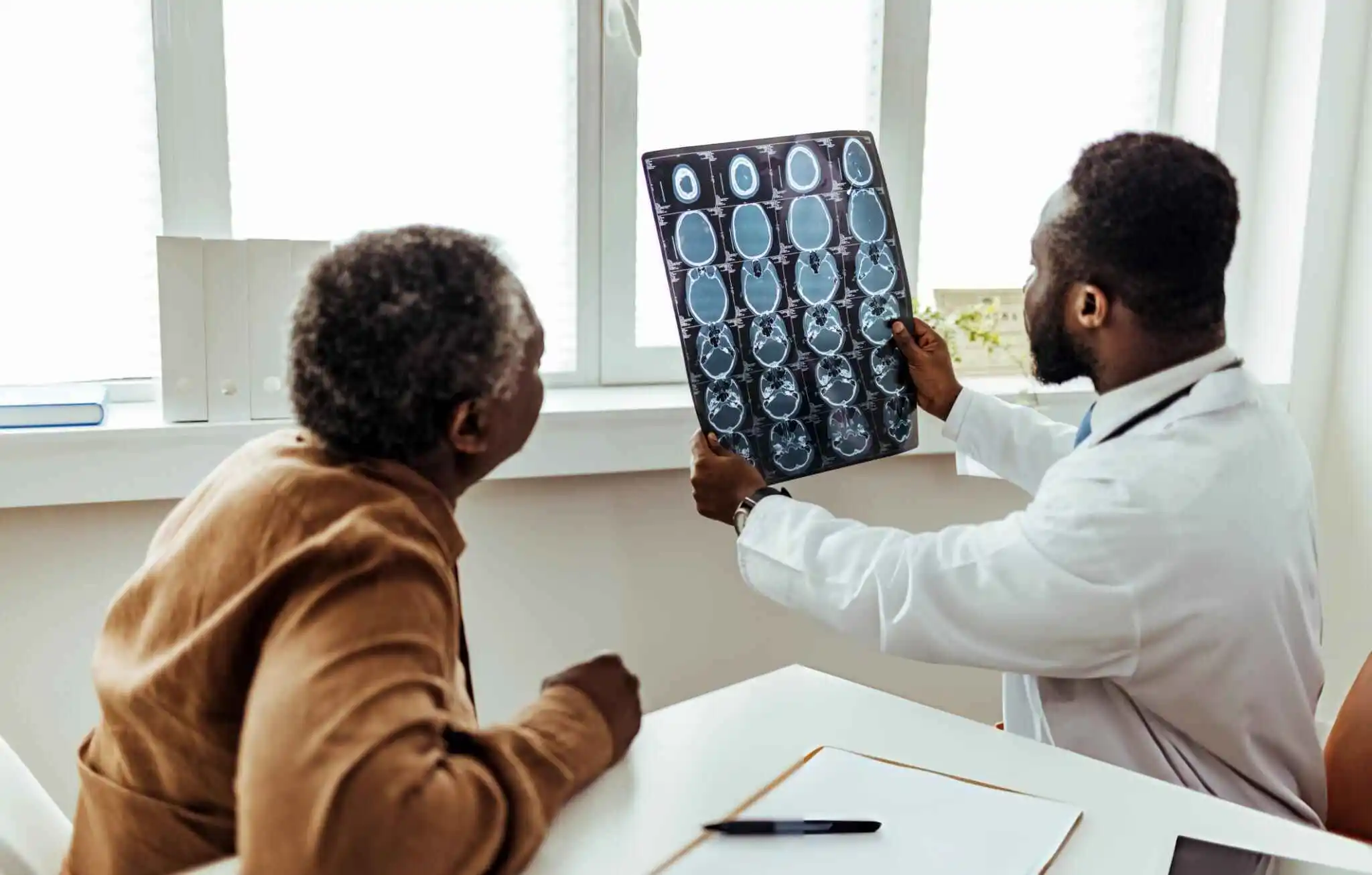
For the past decade, R3 has been successfully treating Migraines and Chronic Headaches with stem cell and exosome procedures. The regenerative biologics are applied directly into the neck and surrounding tissues with direct injections, and also infused through an IV. Depending on each patient’s unique history, R3’s providers may also incorporate an intra-nasal or intrathecal application.
R3’s providers use one to two million stem cells per kilogram, to make sure that patients achieve the absolute best outcome possible. Between 50 and 100 billion exosomes are included with each procedure.
Similar to the research mentioned above, R3 Stem Cell’s outcomes for migraine and chronic headaches have been exceptional! The patient satisfaction rate is 85% year over year. Patients typically experience less headaches with less severity and a reduced need for medications. Keep in mind results cannot be guaranteed and will vary between individuals.
Because stem cell therapy for migraines and chronic headaches is not a permanent cure, it’s important to make it affordable. Repeat therapies can help maintenance and/or achieve additional improvements for pain relief. So a lot of patients seek additional treatments at R3 Stem Cell every twelve to eighteen months.
R3 Stem Cell’s fees are less than half what comparable (and reputable) regenerative clinics charge. Be wary of clinics trying to pass off PRP as a stem cell therapy. If they mention only taking your blood for the treatment, it is NOT a stem cell treatment!
For the past decade, R3 Stem Cell’s Centers globally have performed over 24,000 regenerative procedures in six countries. Several hundred have been for SCI. Patient satisfaction across all conditions treated is 85%!
R3 combines safety, effectiveness and affordability for the therapies. Internationally, the Intellicell is used, which is culturing the most active mesenchymal stem cells to create the “smartest” stem cell in the world!