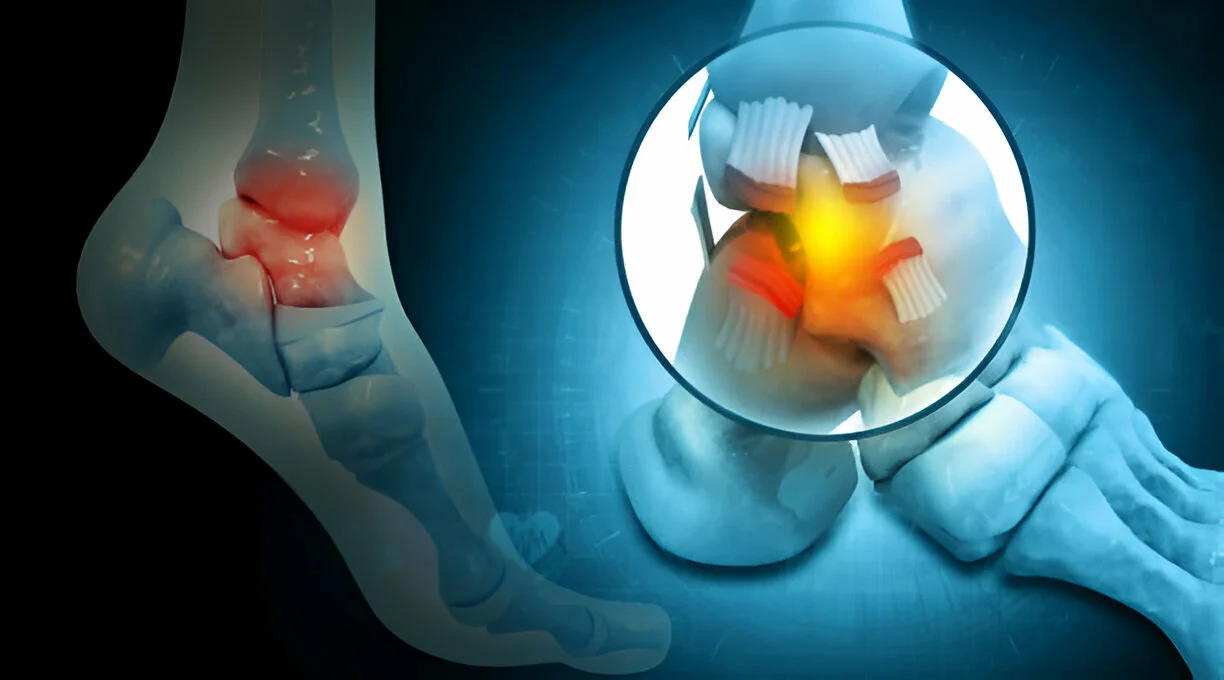
10 Mar Stem Cell for Common Ankle Pain
It can be frustrating when you experience foot or ankle pain because these body parts play a big role in your daily life. Considering how important these body parts are, getting treatments that work and remain effective in the long run is important. If you’re...